For the past few years, the news headlines have been a rollercoaster. First we were dealing with some new COVID-19 virus that turned the world upside down. Then we were worried about murder hornets. What’s next? Apparently, it’s a disease called monkeypox. Seriously? That’s it. I’m out. Do I actually need to be worried about this? Let’s break through some of the news stories and talk about the facts in an understandable way.
What causes monkeypox?
The monkeypox virus is a part of the Orthopoxvirus genus, which hasn’t recently been a cause for concern in humans. But you might have heard of another awful disease in the genus called smallpox. This disease killed over 300 million people between 1900 and its eradication in 1980 thanks to a worldwide vaccine effort. Thankfully, monkeypox isn’t nearly as dangerous. However, it looks similar. I’ll detail the symptoms soon.
Where does monkeypox come from?
Monkeypox isn’t new. It’s existed in central and western African rainforests for many years, but it hasn’t spread globally until recently. The virus is natural in non-human mammals like rodents, squirrels, and, you guessed it, primates. There have been occasional outbreaks in humans, most likely due to people cleaning animals and eating their undercooked meat. This process of transmission from animals to humans is called zoonosis. Hopefully that comes in handy next time you’re watching Jeopardy.
So if it isn’t as deadly as smallpox and cases have been around for years, why are we hearing about it now? Well, even if we’ve seen cases of animal-to-human transmission, we haven’t seen much human-to-human infections until recently. We aren’t sure exactly why, but experts believe a mutation in the virus is the most likely culprit. Now we’ve seen about 50,000 global cases, and around 18,000 have been in the United States.
Am I at risk? How does monkeypox spread?
Monkeypox spreads primarily through skin-to-skin contact with the fluid inside the rash it creates, so thankfully, it’s easier to avoid than something like COVID-19. Some experts are looking into the possibility that it could be spread through respiratory droplets, but the CDC doesn’t think it’s likely.
To narrow the risk factors down further, the majority of cases in the United States have come from gay, bisexual, and other men who have sex with men.
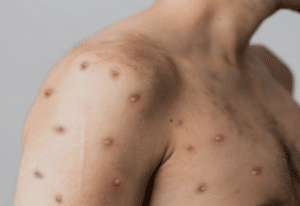
What do monkeypox symptoms look like?
Most of us have probably seen chickenpox before, so that’s the easiest comparison to make.
Monkeypox has no relation to chickenpox beyond its appearance, but if a patient had come to me with these symptoms last year, I probably would have suspected the case to be chickenpox before the test results came back. The blisters are large and painful, and if you see them, it’s important to avoid contact with pregnant women, children and others who have weakened immune systems. Until the blisters scab over and new skin appears, it’s best to avoid contact with anyone.
Can you give me a monkeypox timeline? How does it progress?
The first stage of monkeypox is called the “prodromal phase,” and patients typically exhibit flu-like symptoms. Even today, if a patient came in with a fever, headache, body aches, chills, swollen lymph nodes, etc, we’d check them for COVID, flu, or strep.
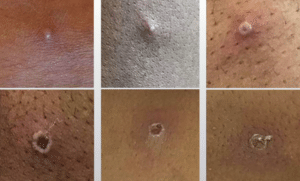
Then, of course, the rashes appeal. The first blister that comes up usually looks like a pimple with a divot in the middle. We call the blisters “vesicles,” and the divot indicates that it’s “umbilicated.” After that, black areas called “eschars” appear around the blister. Maybe those words will come up on Jeopardy too.
Once the scab falls out and new skin is growing, patients are no longer infectious. Until then, stay away.
Given how this virus spreads, it should be pretty obvious if I need to be worried, right?
For the most part, you’re right. You only need to be concerned if you’ve made skin-to-skin contact that breaks a vesicle. However, we still aren’t totally sure that it can’t be spread through airborne fluids, so it’s best to remain masked around infected people and tread carefully.
If I make contact with someone with monkeypox, when should I expect to know if I’m infected?
Monkeypox incubates within a 5-21 day period. If you make contact, you should limit all contact and wear a mask for 21 days. If there’s still no rash after that period, you should be safe. The CDC has broken risk factors into three tiers:
Low Risk – You’ve been around someone with monkeypox for less than three hours Medium risk – You’ve directly made skin-to-skin contact with intact lesions or been
around an infected person for more than three hours
High risk – You’ve made direct, skin-to-skin contact with an infected individual’s broken skin or been near an infected person’s face for three or more hours.
I think I might have monkeypox. What should I do?
You should call your doctor and make an appointment. Let them know you’re concerned about monkeypox and check that they can test for it. At Integrity Urgent Care and Xpress Urgent Care, we’ve already tested for and diagnosed multiple cases.
The test is fairly easy. We’ll swab the infected skin until it opens and send the fluid we collect to the lab for testing. You’ll need to quarantine until the results come back. If it’s positive, we’ll report your case to the health department for contact tracing purposes.
What do I do if I test positive for monkeypox?
I know COVID has probably made you sick of quarantining, but here we go again. You’ll have to isolate as much as possible and wear a mask if you’re in a house with others who can’t stay somewhere else. This will typically last around three weeks, or until your rash scabs over and begins to heal.
Unfortunately, you’ll just have to let the virus run its course. The symptoms are painful, so you can take ibuprofen and Tylenol to help. A few patients may qualify for a new experimental treatment called Tpoxx, but most won’t. Your healthcare provider will let you know if you’re a candidate. If you are, they’ll have to request it from the CDC’s Strategic National Stockpile. These are typically saved for very severe cases with high risks for bad outcomes.
What about the monkeypox vaccine I keep hearing about on tv?
Two vaccines are being used under emergency authorization. If you’ve received a smallpox vaccine, you’re probably already protected. If you’re at a particularly high risk due to frequent exposures to infected people, talk to your healthcare provider about vaccination.
Some people qualify for post exposure prophylaxis (PEP), which means they can get vaccinated after exposure. This process is typically also reserved for high-risk encounters with infected people.
Unfortunately, there is a nation-wide shortage of vaccines, so health departments are being very picky with who can get vaccinated. I’m a provider, and I don’t qualify for the vaccine. I was speaking with an infectious disease doctor a few weeks ago who is a major referral source for positive monkeypox cases, and even she doesn’t qualify for the vaccine. She wears normal clothing with a mask when dealing with monkeypox patients, and she feels this is all that’s necessary.
Should I be worried about monkeypox?
To summarize, monkeypox is a viral disease spread through skin-to-skin contact with infected individuals. We don’t need to be afraid, we just need to be careful. If you’ve been in close contact with someone who tests positive, quarantine for 21 days. If no rash develops, you’re good to go.
If you do become infected, keep in mind that your only course of action is to let it run its course. Quarantine until the scabs fall off and fresh skin grows. A small portion of people are at risk for getting very sick, and those people should be guided through the treatment process. Your healthcare provider can help you understand if that includes you.
Thanks for reading, and feel free to visit any Integrity Urgent Care or Xpress Wellness clinics to get tested if you have a rash. We encourage you to keep making educated healthcare decisions. Let us know if you need help.
Thank you,
Dr. Eddy Dark
Associate Medical Director
Xpress Wellness Urgent Care / Integrity Urgent Care